Pediatric Pulmonary Contusion
Regardless of where you work, you will see injured children. Unintentional injuries far exceed all other causes of Mortality in the pediatric population. Certainly the #1 cause of death after blunt trauma in pediatric patients is Head Injury… but did you know that #2 was Thoracic Injury? And the most common intra-thoracic injury in kids is Pulmonary Contusion.
The pediatric chest wall is very compliant…
- Which is good, because ribs don’t often fracture…
- But it is also bad, because it doesn’t dissipate force, which leads to more of the impact force being directly applied to the lung tissue.
- This force can cause blood to fill the alveoli (Pulmonary Contusion) and that can lead to V/Q mismatch, which in turn leads to hypoxia.
- In addition, the contused lung tissue is now stiffer than before. This, in conjunction with the more compliant chest wall, makes the child’s work of breathing even more difficult.
- The amount of hypoxia and level of respiratory distress will be predicated by the amount of lung volume involved.
So, if we want to know lung volume… is CT scan best determine the patient’s course?
- The simple answer is, “No!”
- CT does define pulmonary contusion earlier than CXR.
- CT does define lung volume involved better than CXR.
- But CXR findings correlate with length of hospital stay, # of ICU days, and # of ventilator days.
- Pulmonary contusion not seen on CXR but picked up on CT is not as significant as pulmonary contusion seen on CXR. If the less sensitive study finds the condition, the condition is likely worse (my simple minded way of thinking of it).
- Furthermore, management is determined by the patient’s clinical picture… not by imaging necessarily.
Management strategies:
- Good pulmonary toilet (Pain control and incentive spirometry).
- Supplemental Oxygen as needed
- Help decrease work of breathing (BiPap may be useful)
- Large contusions are at an increased risk of mechanical ventilation… but if you fluid restrict and use BiPap early, perhaps you can avoid that.
- Some may progress to develop complicating pneumonias… but empiric antibiotics are NOT recommended.
Kwon, et al. CT diagnosis of Pulm Contusion does not correlate with increase mortality. J Ped Surg; 2006 Jan;41(1):78-82


[…] environment! Due to conditions like severe respiratory illness (ex, asthma), acute trauma (ex, pulmonary contusion), or acute metabolic derangements (ex, DKA) children may benefit from endotracheal intubation. We […]
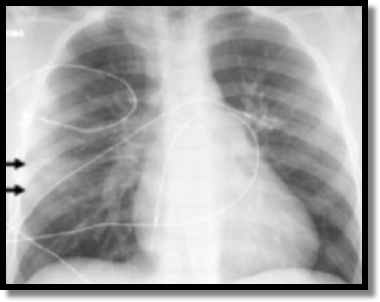
[…] Lung Contusion […]
[…] with managing all aspects of pediatric traumatic injuries (ex, Splenic Injury, Abdominal Trauma, Thoracic Trauma, Aortic Injury, Pelvic Trauma). Recently a colleague of ours @BurnsidePatrick inquired about […]
[…] We have already discussed the most common conditions associated with pediatric thoracic trauma (Pulmonary Contusion and Pneumothorax). We have also covered some procedural strategies for managing the child with a […]