Post-Tonsillectomy Hemorrhage
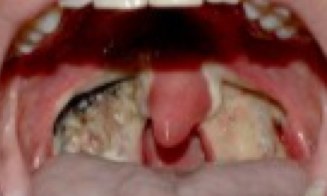
We know that all bleeding eventually stops: ideally, by means that we have imposed rather than by exhaustion of the patient’s RBC resources. We also know that the easiest, and often most efficacious, way to halt bleeding is to put some manual pressure on the source of bleeding. Well, that isn’t always so easy to accomplish. How do you put your finger on a bleeding tonsil? Let’s review Post-Tonsillectomy Hemorrhage.
Tonsillectomy
- Rates of tonsillectomies have decreased slightly over time (it seemed like having tonsils used to be a good reason to have them removed).
- Current reasons for tonsillectomy include:
- Sleep-disordered breathing and sleep apnea
- Tonsillar hypertrophy is most prominent between 3 and 6 years
- Tonsils involute after age 8 in most.
- Children with sleep apnea benefit from tonsillectomy.
- Unfortunately, obese children with sleep-disordered breathing are less often cured by tonsillectomy.
- Severe recurrent sore throats
- It is shown that children have less sore throats after the tonsillectomy.
- It is not proven that this improvement is due to the tonsillectomy though.
- Various other relative indications (ex, Peritonsillar cellulitis/abscess, dental malocclusion, hemorrhagic tonsillitis, prevention of secondary rheumatic fever)
The procedure
-
Tonsillectomy
- Gold Standard (since 1910’s) – used in all major studies
- “Hot” and “cold” techniques
- “en bloc” excision of the entire palatine tonsil and its capsule
- Removes tonsil completely
- Leaves relatively large wound with exposed muscle and bridging blood vessels.
- Glossopharyngeal nerve, fat, tongue base muscles can also be exposed.
-
Tonsillotomy
- Less radical approach, but still majority of US surgeons do the former.
- Removal of only the exophytic portion of the tonsil (“partial tonsillectomy”).
- Reports of slightly less pain and less bleeding compared to other.
-
Typical Healing Course
- Tonsillectomy is very traumatic.
- Edema of the uvula, tonsillar pillars, and tongue is common.
- Within 24hrs a Fibrin clot on the tonsillar fossae develops.
- By the 5th day post-op, the Fibrin clot has proliferated and made a thick cake (that looks terrible).
- Mucosa from the periphery of the wound begin to grow inward and the clot begins to separate from the underlying tissue after ~1week (this is the point when secondary bleeding risk is the highest).
- Wound healing may take ~ 2 weeks.
Post-Tonsillectomy Hemorrhage
- The vascular supply to the tonsil is robust (5 primary arteries).
- The surrounding tissues do not compress upon themselves.
- Tonsillectomy is said to be “the ultimate test of hemostasis.”
- Post-Tonsillectomy hemorrhage rates = 2.5 – 7
- Hemorrhage can lead to shock, airway obstruction, and death (those sound bad).
-
Primary hemorrhage
- Occurs within first 24 hours of the procedure.
- With procedures being done as outpatients, these may present to your ED.
-
Secondary hemorrhage
- Occurs after more than 24 hours from the procedure.
- Most commonly seen at Post-op Days #5 – #10, when the fibrin clot sloughs off.
Management
- Air, Breathing, Circulation (when in doubt, ABCs).
- Assess hemodynamic stability … get access if necessary.
- Inspect the area for signs of hemorrhage or blood blot.
- Most are not actively bleeding on arrival to the ED (yeah!).
- Those who have bleeding or have a visible clot usually are treated with surgery.
- In one study, patients with minor bleeding had a 41% rate of severe bleeding within 24hrs.
- Adolescents and Adults may be treated slightly differently with trials of topical cautery under local anesthesia, but young children often require general anesthesia.
- Those without evidence of bleeding or blood clot formation should be observed to define stability. Any repeated bleeding should be viewed as a warning sign of serious hemorrhage.
Major Bleeding Management
- Mobilize the troops up in the OR.
- Have child lean forward (to help keep blood out of airway).
- Shed lots of light on the subject (headlamp will be vital for you).
- Grab your Magill Forceps and a ton of gauze and suction.
- Try to evacuate as much of the clotted blood as possible so you can get to the tonsillar fossae.
- Now apply direct pressure on the tonsillar fossae with the gauze wrapped around the end of the Magill’s.
- Adding some epinephrine (1:10,000) to the gauze has been shown to help (but I wouldn’t wait around … start with direct pressure).
- Remember to push out laterally onto the tonsillar fossae (do not aim posteriorly).
- Expect that the child will not tolerate this well… consider KETAMINE! (man, I love ketamine!)
- Also, expect that you may need to manage the airway. This will be difficult as once you lay the patient supine all of the blood is going to be in the airway (so ideally you would have some control of the bleeding prior to this… but your job is never as easy as you would like it to be).
- Type and Cross!
References
Isaacson G1. Tonsillectomy care for the pediatrician. Pediatrics. 2012 Aug;130(2):324-34. PMID: 22753552. [PubMed] [Read by QxMD]
Windfuhr JP1, Schloendorff G, Baburi D, Kremer B. Serious post-tonsillectomy hemorrhage with and without lethal outcome in children and adolescents. Int J Pediatr Otorhinolaryngol. 2008 Jul;72(7):1029-40. PMID: 18455808. [PubMed] [Read by QxMD]
Peterson J1, Losek JD. Post-tonsillectomy hemorrhage and pediatric emergency care. Clin Pediatr (Phila). 2004 Jun;43(5):445-8. PMID: 15208749. [PubMed] [Read by QxMD]
Steketee KG1, Reisdorff EJ. Emergency care for posttonsillectomy and postadenoidectomy hemorrhage. Am J Emerg Med. 1995 Sep;13(5):518-23. PMID: 7662054. [PubMed] [Read by QxMD]


Hi, im 34 years old, Singapore. i had 2 episodes of bleeding post tonsillectomy on day 10 and day 11 for around 15-20mins. I am able to stop the bleeding or rather its stopped by itself after a while and i would gargle iced water to soothe my throat. I just want to share that i am glad to find this blog because it is scary to go through this alone, waking up in the middle of the night fearing that i may choke on my own blood. Take care everyone
I am a 20 year old who has had issues with my tonsils since I was little and chronic tonsillitis since December that no antibiotics or steroids could treat. After my surgery, I had a scab fall off on day 10 while eating ice cream, which busted an artery. Blood shot out so fast you could hear it and and it got everywhere. I was rushed to the hospital and on the way it started clotting. I had a potato sized blood clot filling my mouth/throat. It was blocking my airway, but every time they tried to touch it, more blood would shoot out. They rushed me to the OR and fixed everything in a second surgery and I had to be hospitalized for a few days. Today is day 10 after the second surgery (20 days after the first), and I’m still only able to eat mostly liquids and some pudding consistencies. Also, I have had a horrible case of thrush since day 2, unable to be controlled with three rounds of medicine. Now looking at home remedies for that. Frustrated would be an understatement for me. But I am a red head, and have more sensitivities/reactions to everything. I will say I now have anxiety/fear about bleeding again, making eating and drinking extremely difficult for me. I am traumatized by my bleeding experience, but I’m looking forward to the day I am healed and can eat again.
In 1980 at age 17, after a story like yours, Kaylee, with chronic childhood illnesses, I had a tonsillectomy under general anesthesia. The medical profession was starting to frown on doing so many tonsillectomies, but the many specialists my parents took me to were out of options. I was constantly sick and anemic. After surgery, when no one put an ice pack on my neck, I awakened vomiting copious amounts of blood over the edge of the bed, but whatever came after, I have absolutely no recollection. I healed painfully but uneventfully from surgery but continued on the path of chronic illness until age 48 when a duodenal biopsy showed I had celiac disease. ENTs know nothing about celiac.
Anemia is a common celiac symptom that might clue more doctors today. If your general health is still poor, Kaylee, you might look (with help from a gastroenterologist) into whether celiac could be contributing.
Thanks so much, Dr Fox, for helping me possibly understand an episode of my life that’s still a bit traumatic. That I could have died from unnecessary surgery is just the icing on the cake!
By the way, since going GF eight years ago, I’ve had one brief cold!
[…] Pediatric EM Morsels: Post-Tonsillectomy Hemorrhage […]
[…] Pediatric EM Morsels: Post-tonsillectomy hemorrhage […]
Hello, I am Day 12 post op and have done really well overall. I had some bleeding yesterday from the last little scabs coming off. At that time I did swallow blood not an enormous amount and was in contact with my doctor. My question is can you bleed lower into your throat where you cannot taste, see, or feel that you are bleeding. My stomach hurts quite bad today and I have had no bleeding for over 18 hours.
I had extreme bleeding on day 6 & 7 where clots were forming in my throat blocking my airway until I wrenched hard lung to bring up a ping pong ball sized clott,
To answer you quester when I went to pass bowel movements the next days it was completely dark red / black clotted blood,
I’m not a professional but going on this logic I’d say check your stool for signs of blood as an indication that your bleeding in to you gut,
Best regards,
Luca
I had a bleeding on Day 8… it was at night, a big scab fell off and boom i Just felt the blood dripping to my mouth, since I have anxiety I surely wasnt calm and that made more blood come out. I made it stop after like 2 mins by gargling ice water. I still went to the ER…. when i was waiting for my turn I started bleeding again, everytime i swallowed it oozed more blood… so again i tried to calm down and it eventually stopped. The doctor on call checked my tonsils and gave me medicine to stop further bleeding. Yesterday it bled a little because the clot fell off but so far so good. My ENT hasnt been in town so im not able to see him until Monday…
Will I be okay? everything seems okay in my tonsil beds only the red spot from the bleed…
I have a small blood clot right now from a scab falling off from a yawn. My surgeon said it will go away on it’s own. but what happened in your case? Did the small clot just fall off after a few days like a scab? Or will it be here for a few weeks?
my 17 year old daughter bleeding after 12 day tonsillectomy righ side, what shall i do?
While I, obviously, cannot give specific and individual medical advice… any patient who has post-operative bleeding, even 12 days later, should contact their surgeon to discuss options.
Hope you daughter is well,
sean
Hello, its my 7th day after my surgery and now i have started bleeding every moring although it stops quickly, whats causing it? And is thier any solution for it?
Hello!
Obviously I cannot give out specific, individual medical advice online; however, I would tell anyone who has had a tonsillectomy who now has some (even a little) bleeding to contact her/his surgeon to discuss being evaluated.
Hope you continue to do well,
sean
Hi, I’m on day 12 of post tonsillectomy. I had a bad bleed day 9, went to the hospital and had to go to the OR room to get my left side re-cauterized. I’m feeling ok now, barely any pain. I’m just wondering what are the chances of me getting another bleed? The EMT told me to stay on a soft food diet for another 2 weeks. I’m just scared it’s going to happen again. I’m traumatized. I have a somewhat labour job. Will I be fit to return in 8 days?
I am very thankful for your outstanding post which I review whenever I think of the the possibility of serious post op tonsillectomy bleeding.
One of my concerns is the inability to intubate because of all the blood – Anesthetic Challenges and Hazards of Pediatric Post Tonsillectomy Hemorrhage.
What about attempting finger intubation attempting to palpate the glottic opening and insert the tube on top of your finger when you can’t visualize the opening?
Is that reasonable? I’ve never done it but it was mentioned in a PALS course I took some years ago.
Dr. Wade,
Thank you for your appreciation of the Morsels!
As for digital intubation… I have seen it used once, in an adult, while I was a resident by one of the most heroic EM doctors I trained with… and would still consider it to be a heroic feat!
Overall, I would say that with direct pressure and suction, you should be able to clear your way to visualize the glottic opening and would prefer direct visualization over blind, digital intubation. While I do like to use videoscopic laryngoscopes primarily, this would be one occasion that I may grab my trusty, dusty cold steel blade.
That being said, sometimes things just don’t go your way (we’ve all been there when that happens)… so having alternative strategies is imperative. I would likely go for transtracheal ventilation (see separate Morsel and Procedure Video) first in that “can’t intubate, can’t ventilate” scenario. BUT, having an additional strategy to get the result you want, I think is reasonable.
Thank you,
sean
I’m 22 years old, Male, and had my Tonsils out on 9/7/17. 4 days in I had some bleeding, did as prescribed, gargled cold water and spat, repeated until it stopped, got the bleeding controlled under two minutes, then called my doctor. The next day I saw my surgeon to check-in. The day after (two days after the first bleed) things took a turn, had a slow bleed, as I was attempting the same treatment out of nowhere the clot ruptured causing an extreme hemorrhage. It made the first bleed look like nothing. As soon as the hemorrhage occurred I attempted to gargle cold water and spit, the problem became that it was bleeding so profusely that by the time I’d spit the blood and tilted my head back to gargle, my mouth and throat where already full again and I began choking and coughing. At this point I just started rinsing and spitting as fast as possible to avoid choking and hoping that the cold water would at least do something. Then I tried really focusing to see if I could slow my heart rate a bit in the hopes that would slow the bleeding enough to give me a chance to gargle. Not sure if it worked but eventually the bleeding did slow. During the bleed I ended up coughing up the clot in bits. Now initially my first instinct was to call 911 because I live almost an hour from the nearest hospital but as things were I just couldn’t get to my phone. So I stayed at the sink hoping for the best. After about twenty minutes I got the bleeding under control and was able to gargle cold water and stop it almost completely. All that was left was a small slow bleeder that was too low in my throat to reach with gargling water. Luckily I was staying with a family member for my recovery, after I got things under control I let her know what happened and she was able to drive me to the ER. By the time I got there my legs and arms were starting to go numb, managed to run inside, shirt covered in blood, they got the message from the imagery, they quickly grabbed a wheel chair and brought me to the ICU while my family member gave them the details of what happened and the surgery. In the ICU they gave me a number of IV medications, including Tranexamic Acid (TXA) to stop/prevent bleeding and also an anti-nausea med to prevent vomiting. I stayed in the ICU for 4 hours, the ER Doctor said he wanted to hold me for 24 hours of observation, then my Surgeon showed up to check things out and informed me if there was any further bleeding during my stay she’d come in and I’d be sent to the OR to re-cauterize the surgical site.
I learned a few things from this episode. First, keep your phone on your person at all times so you can contact help if things go sideways. Second, staying collected and thinking through the problem is important, I dunno if it actually physically helped but I’m sure it didn’t hurt, just gotta stay focused and deal with it as it comes. Third, it really is important to have someone else on the premises who can either contact 911 for you or drive you to the ER in an emergency.
Had I failed to gain control of the situation and lost consciousness I don’t know what would have happened. I know I wouldn’t have been checked on until that evening, (I’m typically left alone to sleep in the morning and it was 6:30 am when this all occurred, so I would have presumably been on the floor for at least 12 hours if not more before being found).
Anyhow, as of this writing I’m still at the Hospital completing the observation period. Things are looking good, as long as I get through the night without bleeding I won’t have to go round 2 in the OR.
I hope whoever reads this can take away a few of the above lessons, primarily about the phone, the feeling of having no options and trying to beat the blood loss before it beats you is not a fun one, so learn from my mistake, when recovering always have a means within arms reach of getting help.
Best,
Paul
I am 14 days post op T&A. I am 27. I just got my eleventh hemorrhage to stop. That’s right, eleventh. First occurred POD 3 on the left. Then 1-2 times daily POD 7-14. Each bleed is a gusher. The left was cauterized under local in the ED POD 7. However, the right has been difficult to tame. After three ED trips and one F/U with ENT to no avail of finding the troublesome vessel I just take care of it at home hovered over the sink until it slows enough that I can drink/swish ice water. It feels like I’m going to choke to death on my own blood every time it happens. How long post operatively is the risk for bleeding?
Hi again, I just wanted to see if you saw my questions from the last comment. Thank you for any answers you may have.
Chris,
I am sorry your family has been through such an ordeal.
Naturally, I cannot comment on any particular surgeon and her/his proficiency. What I can say is that bleeding after tonsillectomy is common! This is why I wrote the post to help Emergency Care clinicians provide optimal care when it does become an issue.
If you are not comfortable with a physician, any physician, it is your right to seek care with another provider.
It is also possible that there is an underlying bleeding disorder, but that should be brought to the attention of your primary care provider.
I hope that this helps… and that your family doesn’t have to go through this again.
-sean
Hi there,
I’m so grateful that I came across this post and the comments to know that we are not alone in this. My son is 3 years old and had a tonsillectomy due to having strep throat infections 5 times since August. (His older brother also had his tonsils removed at age 3, but for obstructive sleep apnea and had no complications recovering.) His surgery was on December 27. Early January 2 (Day 6), he had his first bleeding. He woke up in the middle of the night panicking and screaming and then started showing signs of blood in his mouth about 5 minutes afterwards. We gargled with ice water and got it to stop. When looking at his throat, I could see what I now know was a clot on the right side. After resting for 20 minutes and talking with the doctor on the phone, he threw up what I would amount to a cereal bowl-full of blood and clots and we headed to the ER. Walking into the ER, he threw up 3 more times, of similar amounts as before. He had a cautery surgery and we went home shortly after surgery. Day 7 had no bleeding. Day 8, in the early hours, we had another bleed. A mouth full of blood but we were able to get it to stop with ice water. We saw the ENT once the office opened for a professional look. He saw no active bleeding. The early hours of Day 9, we had 3 bleeds at midnight, 4am, and 8am – all big mouthfuls of blood. Each time we were able to get it to stop with ice water after about 10 minutes. We came into the ENT office again and he saw some “oozing”. We were going to take a wait-and-see approach to determine if we needed to go to the OR again. A few minutes later, he threw up again a large bowl-full of blood and the ENT met us promptly at the hospital and performed another cautery. Before the surgery his hematocrit was 24 (baseline numbers from the pediatrician were 36). The ENT ran some coagulation studies to determine if the bleeding was from a clotting issue and the blood for those tests had his hematocrit at 15. We spent the night at Children’s Hospital where he received a blood transfusion bringing his hematocrit back up to 24 (day 10). On Monday, Day 13, his hematocrit was 26.8 checked by his pediatrician. On Thursday, Day 17, he had his ENT follow up and the ENT said that he doesn’t expect any more bleeding, but to still not get his heart rate up with any activity and that he can return to school next week.
I have several concerns and questions:
1. Our ENT said 1:100 will bleed following a tonsillectomy. How common is this to have TWO cauteries following a tonsillectomy?
2. My two oldest sons are 4th generation tonsillectomy patients. I have one more son who is 18 months old. How likely is he to have similar bleeding complications should he also require a tonsillectomy?
3. And the elephant in the room: I realize even the best surgeons have “off” days and mistakes. How likely is this surgeon error?
4. Would you recommend the same ENT doctor or switching if my youngest son required a tonsillectomy in the future?
My daughter had a tonsillectomy on 12/2/16 and Her first post op bleed 12/9/16 from the right side. The ENT was available and cauterized it. Seven days later 12/16/16, the left side bled and had to be cauterized. The problem I am having is that it keeps bleeding. We are able to stop it with ice water, but she bleeds about 16-20 minutes before we stop it. We rushed to the ER twice and in both incidences, she had stopped bleeding by the time we got there, so it didn’t look like we had a real emergency. On the 2nd ER visit, her hemoglobin had dropped a little. I am really concerned. Any advice?
I’m sorry to hear of your struggle. I would recommend seeing your ENT surgeon again.
I am a medical student. Exactly what are the five primary arteries that perfuse the tonsillar fossa, and which one is most likely to rupture?
Elaine,
Unsure about which most likely to bleed, but I imagine it doesn’t likely matter.
The five arteries are:
1) one branch off of the Lingual artery
2) one branch off of the Maxillary artery
3) one branch off of the Carotid artery
4+5) two branches off of the Facial artery
Excellent, what a weblog it is! This blog presents valuable data to us, keep it up.
My son had 2 post op bleeds after day 12!
How many days apart was the 2 bleeds or how long between them
I’m the worried mom of an 8 year old boy. Day 9 after T & A removal, he bled 2 times during the day, we were able to stop it with ice etc. That night he bled so much, and so much of it went into his stomach he woke up throwing up several pints of blood and nearly passed out when totally pale. After observation with IV in the hospital after calling 911 our ENT said he could go home. Day 11 he started to bleed again, slow steady stream. We were able to stop it. After talking to ENT again via phone, he said, to observe more, if it starts again the only option is to put him under and cauterize it. Should I be worried? I don’t want to be pushy or crazy, but I don’t want to put my child at any risk. I’m sleeping with him every night to make sure he’s okay. Once bitten twice shy sort of thing. The only thing that keeps running in my mind, is when the Dr and nurse said that his adnoids were REALLY, REALLY large and they had to go further back to get it all, and that they were happy he had them out (for apnea reasons and recurring strep) So of course I found your site with the “let me be the Dr. Google” Thank you!
I’m sorry that you are going through this now, but know that you are not alone as this is a common issue after tonsillectomy.
Given that bleeding can occur even after 1.5-2 weeks post-op, what you describe does require attention. That may be more observation or may be cauterization. Given that this is the Internet and I am not your doctor, I cannot give you real advice, but would encourage you to continue to keep your ENT surgeon informed and perhaps even advocate for a repeat examination.
Hope that that helps,
Sean
Erin, how is your son doing now? My 8 year old is going to have surgery tomorrow and I’m worried of course. And how were you able to stop the bleeding?
Hi Becci, I’m sorry I didn’t see this. After all that fun, he was done bleeding, we definitely kept him out of P.E and games with friends for a long while after that at least another 2 weeks minimum. But he is amazing now. Would I do it again…100% Yes. He is a new little boy. He can run longer without getting short-winded. Hasn’t had Strep or a sinus infections at all since then, even when his friends have been sick. He didn’t get sick all winter except for a tiny cold, which is WAY not the norm for him. He had to get used to speaking differently though. I think that since I went into this surgery very worried, I was ready for something to happen, but no one can ever be totally prepared. I really admire our ENT, he was always on hand, and even gave me his cell phone number and checked in with us on his own after the first incident. Being such an anti-surgery mom, this is the first time someone has cut into my boy, not even circumcision, but this was indeed a necessity for him. He looks back now and is also happy he had it done, and he loved being in the ER for the bleeding, he got real good treatment and “had cheesecake!” So all it well. How was your sons surgery?
Tonight I had 18-year-old who had some pretty decent bleeding on post op day five after tonsillectomy. There was a big clot sitting on the right tonsil it was make me feel pretty uncomfortable. Wasn’t too sure about management and Up-to-Date was worthless, so I went to Dr. Google. Dr. Google sent me directly to the Ped EM Morsels on post tonsillectomy bleeding, which was, of course, incredibly helpful. Wanted to take the opportunity to give you a shout out.
-Dr. Kammer
Dr. Kammer,
Thank you so much for the feedback! I am glad that the PedEM Morsels have assisted you in your time of need.
If there is ever a topic that you would find to be helpful for the Morsels to cover, feel free to let me know and I will see what I can do.
Have a great day,
sean
[…] the audience (you all) who read these Morsels love critical care topics (Post-Tonsillectomy Hemorrhage has been the most viewed Morsel since it was written in 2012), but excellent care in the Peds ED […]
[…] topics in the Ped EM Morsels over the past numerous years. Many are quite attention grabbing (ex, Tonsillectomy Hemorrhage, Delayed Sequence Intubation, and Submersion Injuries, and Lawn Mower Injuries), but that does not […]
[…] following is a link to the excellent blog post Peds EM Morsels Post-Tonsillectomy Hemorrhage. It covers what to do for the patient with massive post op tonsillectomy […]
[…] catches your attention in the Peds ED (or any ED for that matter). We have previously covered Post-Tonsillectomy Hemorrhage, oropharyngeal trauma, Hemorrhagic Disease of the Newborn, ITP and the significance of Wet […]