Traumatic Pneumothorax
We all know that kids are not little adults (seriously, how many times can we hear that?), but when we consider procedures it important to appreciate that there are differences. The most important being that EVERYTHING is just smaller, which makes your job more difficult.
When a pneumothorax needs to be dealt with on an adult patient, we find great comfort when we insert our finger into the thoracic cavity and feel the squishy lung (YES! I am not in the abdomen! Sweet!); however, that same reassurance will not likely be obtained in a pediatric patient, because you simply cannot fit your finger between the ribs. Additionally, the narrow intercostal space also exposes the neurovascular bundle making complications more likely. So, what shall we do?
First of all, is this in need of an emergent procedure?
- The pediatric patient’s more mobile mediastinum coupled with the fact that intrathoracic pressures are more readily transmitted to the right atrium will make them more likely to have decreased cardiac output (from impared preload) or outright tension physiology.
- Fortunately, emergent thoracostomy is rarely required in children. Most can be done in a more controlled setting, which will help avoid complications.
Next, is a procedure needed at all?
- Conservative / Non-operative Management is appropriate for:
- Stable patient with no evidence of respiratory distress.
- Small pneumothoraces (some have said up to 20%, but no good pediatric studies that define a predictive volume).
- Not in need of positive pressure ventilation (although some studies have shown no change in outcome with small pneumothoraces and positive pressure ventilation).
- Consider transport method… transport by high-altitude flying aircraft may cause pneumothorax to increase in size.
- For the stable patient with small, asymptomatic pneumothorax Observation or Aspiration may be appropriate.
- Aspiration (not decompression of a Tension Ptx) is relatively easy to do (see video) and doesn’t need to be followed by a chest tube.
- If the ptx reaccumulates, then a chest tube would be warranted.
Finally, if you decide a chest tube needs to be placed… be Humane!
- Naturally, give appropiate analgesics and involve distraction techniques / child life!
- Pick the smallest tube that will do the job!
- Pigtail cathethers (see video)
- Pigtail cathethers can adequately drain air and non-viscous blood.
- Placement is better tolerated and their presence in the chest wall is better tolerated.
- Ultrasound can be used for guidance.
- Thoracostomy tube
- Would be necessary if you are concerned for more viscous substances (pus and thick blood).
- You can still choose a humane size!
- Pigtail cathethers (see video)


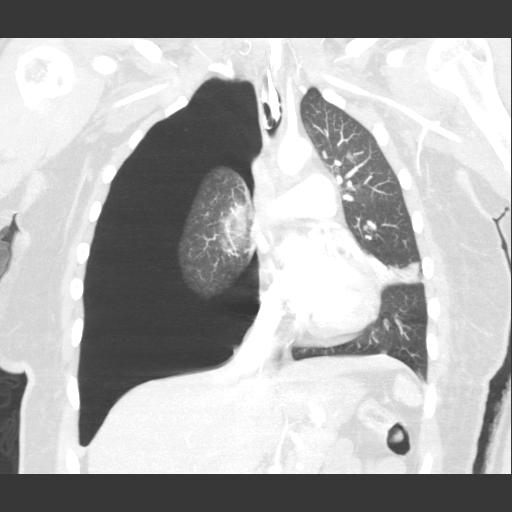
[…] Pneumothorax […]
[…] mortality in children. Appropriately, we have discussed numerous topics pertaining to trauma (ex, Pneumothorax, Traumatic Aortic Injury, Major Brain Injury, Abdominal Trauma) and recently even touched upon the […]
[…] of the differences in anatomy and physiology (ex, Sinus Bradycardia, Aortic Trauma, Back Pain, Traumatic Pneumothorax). What is equally important to remember is that within the pediatric population as a whole, there […]