Mono
Your patient has a sore throat. You have entertained a variety of conditions, including strep pharyngitis and even gone so far as considering Lemierre’s Syndrome, but now really believe that this is Infectious Mononucleosis (IM). What should you know?
Mono Basics
• IM most commonly is seen during primary EBV infection which occurs around 2nd decade of life (highest incidence is in15-24yrs olds).
• EBV is transmitted via exposure to infected saliva (Kissing Disease) and has an incubation of 30-50 Days!
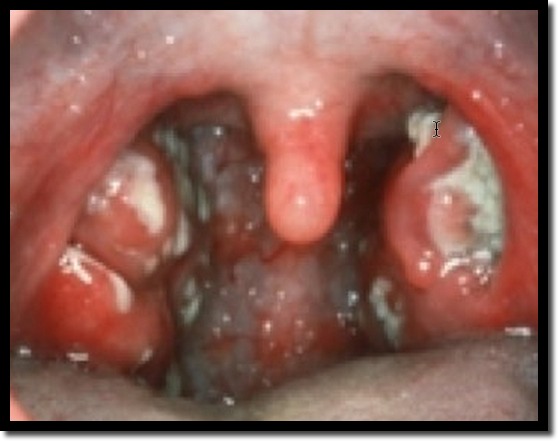
• Classic triad = Subacute Pharyngitis, Fever, and Lymphadenopathy. Malaise is also a significant feature.
• Splenomegaly is often present on ultrasound, but found only variably on exam (15-65% of cases).
• Majority of patients recover without any sequelae… but it may take up to 2-3 months for malaise to fully resolve.
Mono Complications
• Uncommon, but significant complications include (but not limited to):
o Hemolytic Anemia
o Thrombocytopenia
o Aplastic Anemia
o TTP/HUS/DIC
o Guillain-Barre Syndrome
o Bell’s Palsy
o Aseptic Menigitis
o Transverse Myelitis
o Peripheral Neuritis
And the one we all worry about…
o Splenic Rupture (in 0.5-1% of cases) – most occurring within 3 weeks of the diagnosis. Avoidance of contact sports is recommended for at least 3 weeks.
Diagnosis:
o Clinical picture
o Laboratory-studies that support it:
• Absolute and Atypical Lymphocytosis and a Positive Heterophile (MonoSpot) antibody test.
• Monospot tests can be falsely negative in 25% of patients with IM in the 1st week of infection and in 5-10% after the 2nd week.
My take on it all…
- In the ED, patients are likely presenting in a period of time that a definitive diagnosis is difficult to make. Get comfortable with that.
- The Monospot test isn’t that reliable when I am seeing the patient and, more importantly, it doesn’t often change what I am going to do; so I do not generally order MonoSpot tests from the ED.
- Moreover, I have been taught that the WBC is “the last bastion of the intellectually destitute” so I rarely order a WBC to work up an ill-defined sore throat.
- In addition, all of the uncommon, but serious complications will likely present in a more conspicuous manner.
THE SPLEEN
- So then it becomes an issue of the spleen… we all fear the spleen!
- If the patient has a sore throat, I attempt to palpate the spleen. Knowing that the risk of rupture is low, I still have the conversation with the family and stress the need to follow up with their primary.
- If their symptoms of sore throat and malaise are persistent, then the primary care physician will be able to order a Monospot and likely have it be more meaningful than when I saw the child during the first few days of the illness.More importantly is the fact that if you are really considering IM, then early HIV infection should also be on your DDx list. Not to suggest HIV testing be done from the ED, but rather reinforce the need to be able to keep your DDx open and educate your patients and their families that there may be other entities responsible for the swollen lymph nodes and malaise.Once again, my humble opinion… and I welcome your comments and disagreements.


[…] associated with recent, antecedent illness (ex, Mono), although cases noted to follow trauma, surgery, pregnancy, and immunizations. [Pavlik, […]
[…] issues. Many issues are common and often benign, like “sore throat” (ex, Strep pharyngitis, Mono). Other issues can be much more ominous, like “pain in neck” (ex, C-spine clearance, […]
[…] your attention. Most often the parental concern is over whether this is due to Strep Throat or Mono. Naturally, there are a variety of other issues that we must consider. Perhaps this is merely a […]