Perichondritis of the Ear in Children
This is the 601st Ped EM Morsel! Having authored 575 (well, now 576) of them, I am often quite convinced that there are no new topics to discuss. Then July happens and we get 14 more amazing interns who help educate me and remind me that there is always more to learn. Recently, Dr. Teresa Crow encountered an important topic in children that deserves its own Morsel. We have previously discussed several Ear-related issues (AOM, Otitis Externa, Auricular FBs, and Auricular Lacerations). Now let’s review what Dr. Crow was concerned about – Perichondritis of the Ear in Children:
Perichondritis of the Ear: Basics
- Anatomy Matters
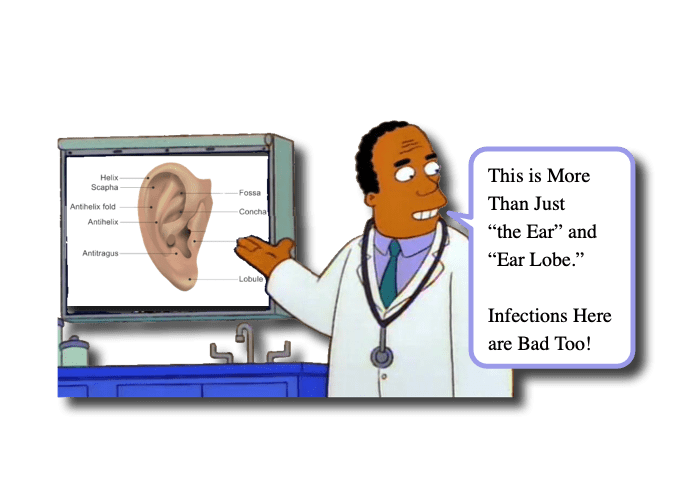
- The external ear is the pinna or auricle and includes the:
- Helix and Antihelix,
- Scapha
- Tragus and antitragus,
- Concha, and
- Lobule
- Cartilage is a prominent and important structure of the superior portions of the pinna (not the lobule).
- The external ear is the pinna or auricle and includes the:
- Auricular Perichondritis = infection or inflammation of the cartilaginous section of external ear
- Risk Factors: [Kim, 2022; Rivera-Morales, 2020; Stewart, 2006]
- High Ear Piercing (ex, through Helix, Antihelix, or Scapha)
- Lacerations
- Blunt Trauma (and hematoma formation)
- Burns
- “Bug Bites” and Digital Trauma (ie, scratching)
- Iatrogenic
- Complications: [Kim, 2022; Rivera-Morales, 2020]
- Focal Liquefactive Cartilage Necrosis
- Permanent Deformity of the External Ear (ie, “Cauliflower ear”)
- The Bugs: [Kim, 2022; Rivera-Morales, 2020; Stewart, 2006]
- Suppurative (with Abscess) Infection:
- Pseudomonas aeruginosa = most common
- Staphylococcus aures
- Streptococcus pyogenes
- E. Coli
- Proteus species
- Non-Abscess infection:
- Staphylococcus aures = the most common
- Pseudomonas aeruginosa and others still may be seen
- Suppurative (with Abscess) Infection:
Perichondritis of the Ear: Presentation
- Redness, Pain, and Swelling of the pinna
- Typically spares the lobule!
- Has normal external auditory canal and TM.
- Other considerations:
- Malignant Otitis Externa
- Mastoiditis
- Auricular Hematoma
Perichondritis of the Ear: Management
- Empiric antibiotics!
- With prevalence of Pseudomonas aeruginosa many recommend empiric anti-peudomonal coverage.
- Some have noted that if there is not an abscess, Pseudomonas aeruginosa is less likely and one could try Staph/Strep coverage at first and watch closely.
- There is often describe concern for the use of Fluoroquinolones in children… but the AAP has noted that there is “no compelling published evidence“ to prevent using them in children in appropriate situations.
- There is increasing resistance patterns though, so it is best to select your antibiotics keeping in mind your local resistance patterns.
- Inpatient Vs Outpatient Therapy
- No standard approach… but… here is what I say:
- “Always Fear Infections in the Hands, Feet, or Face.”
- Those areas have very important and delicate structures.
- Infections there become complicated very quickly and the outcomes can be very poor.
- If treated as an outpatient, may be best to cover with anti-pseudomonas (Ciprofloxacin) antibiotic from the beginning.
- Increasing resistance does make treatment failure of greater concern (which is why some recommend inpatient treatment to start with).
- Close observation is critical (so if discharging, ensure the patient can be seen in the next 12-24 hrs.
- Consult your Friendly ENT Surgeon.
- Even if abscess has not formed yet, they should be involved to help monitor and determine whether drainage will become necessary.
Moral of the Morsel
- The Ear Is Complex! A “minor skin” infection can become a major problem.
- Pseudomonas aeruginosa is like an evil supervillain. Cipro may be the hero!
- Observe to Ensure! Close follow-up or outright admission is needed to ensure this does not become a permanent deformity!
References:
Kim MM, Goldman RD. Ear-piercing complications in children and adolescents. Can Fam Physician. 2022 Sep;68(9):661-663. doi: 10.46747/cfp.6809661. PMID: 36100383; PMCID: PMC9470180.
Rivera-Morales MD, Rodríguez-Belén JL, Vera A, Ganti L. Perichondritis: Not All Ear Pain Is Otitis. Cureus. 2020 Oct 24;12(10):e11141. doi: 10.7759/cureus.11141. PMID: 33251051; PMCID: PMC7686808.
Stewart GM, Thorp A, Brown L. Perichondritis–a complication of high ear piercing. Pediatr Emerg Care. 2006 Dec;22(12):804-6. doi: 10.1097/01.pec.0000248687.96433.63. PMID: 17198212.

